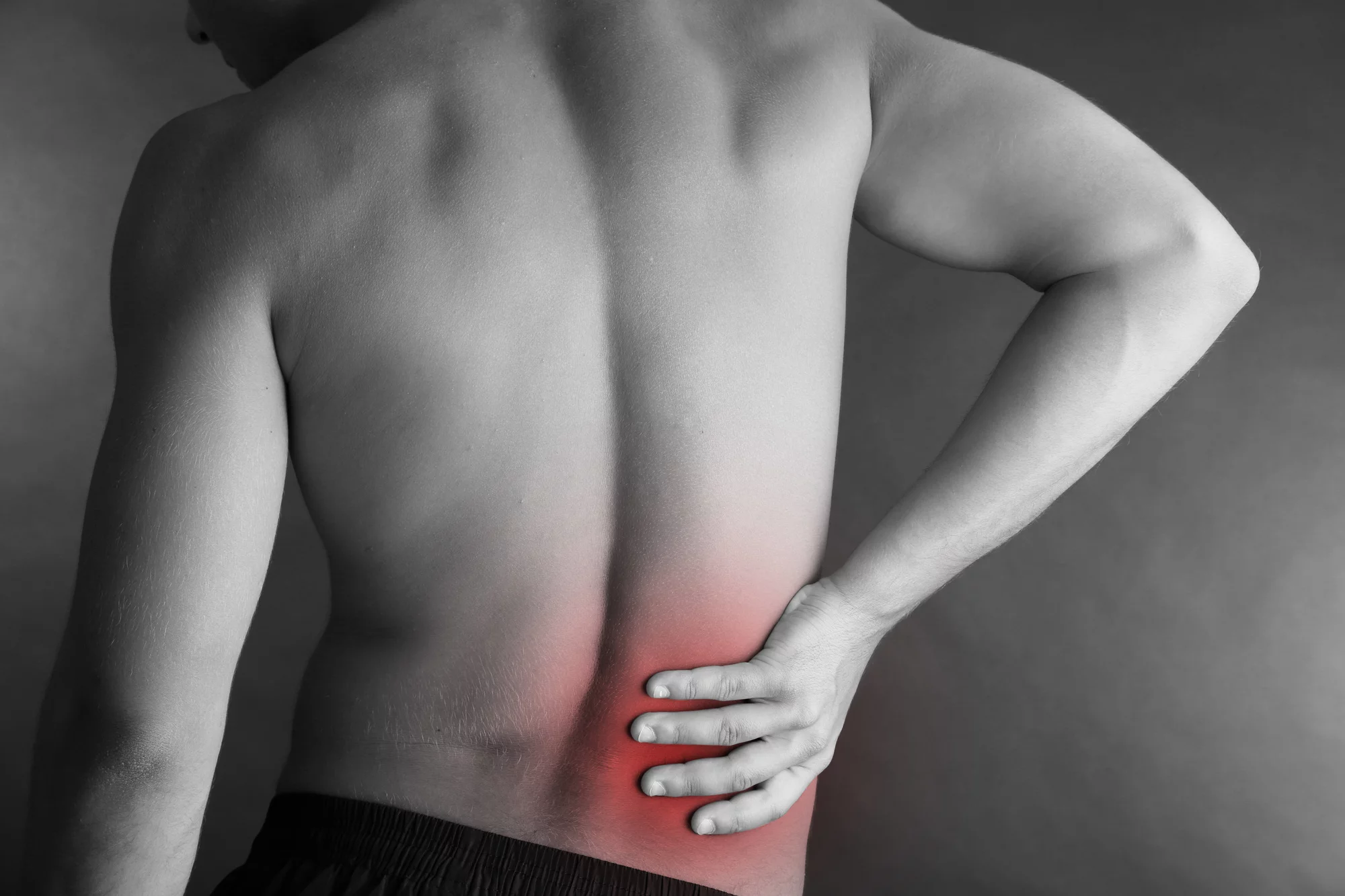
How to Tell if Your Pain is Caused by an Annular Tear
Unfortunately for us, most people suffer from some type of back pain at some point in their lives. In fact, 80% of people will have back pain at some point, and it’s the leading cause of disability worldwide.
But there’s a difference between a sore back after hunching over your computer all day and a serious back injury. An annular tear is one type of back injury that you shouldn’t ignore.
But how can you tell whether your back pain is the result of an annular tear or if it’s just sore because you slept funny on your mother-in-law’s guest bed?
We’re going to go over exactly what an annular tear is, how you can tell if that’s what you have, and what you can do to treat your symptoms.
What Is an Annular Tear?
Our spines are made up of bones called vertebrae. In between the vertebrae are discs that help to protect and cushion the bones. This cushioning helps them to absorb any large shocks or pressure applied to the spine as well as distribute the pressure/weight on our back evenly to avoid one part of the back taking too much weight.
These discs are made of two distinct materials. One part is a soft, gel-like fluid that serves as the cushion.
The other part of the disc is made of something called annulus fibrosus. These are strong fibers that hold the disc together and keep them in place.
An annular tear is when these fibers, well, tear. These tears can be minor and small at the beginning with little to no symptoms. However, they get progressively worse, which can lead to the inner “gel” of the disc to leak out.
When this happens, the nerves in the spine can be impacts, which leads to a great deal of pain.
What Causes Annular Tears?
Most annular tears occur in the lumbar spine, which is a fancy way of saying the lower back. While it’s not impossible for them to happen in other parts of the spine, they’re most common in the lower back.
But what causes this to happen? One of the main causes is something we can’t do much about aging.
As we get older, normal wear and tear lead to parts of our body to weaken. This includes the parts of our back like the vertebrae and the discs. When these parts get weaker, it’s easier for injuries like tears to occur.
There are other factors that can lead to annular tears. If you’re overweight or obese, you’re at a higher risk of an annular tear. The extra weight puts excess pressure and weight on the spine, which leads to tears.
Annular tears can also be the result of accidents, especially ones with sudden or jarring movement of your weight. This could be a car accident, a sports injury, or even just lifting a heavy box incorrectly. When you combine these physical activities with age or obesity, you’re at a much higher risk.
Symptoms of an Annular Tear
Minor or small annular tears usually have no symptoms. However, as the tear gets bigger, symptoms will begin to appear.
The main symptom of annular tears is pain. You’ll have pain in your back that could radiate from the point of the tear to other parts of your back. You may also experience pain in your legs as well.
Difficulty Sitting And/Or Standing
We use our back for almost every movement or activity, even if you don’t realize it. Because of this, you may have trouble getting any relief at all when you have an annular tear.
Even sitting or standing can be very painful.
Consistent Symptoms
As we said before, we use our back all the time. This means that pretty much no matter what you’re doing, you’re going to still have pain if you have an annular tear.
Doesn’t matter if you’re on a hike, sitting in your car, or laying down on a fluffy soft bed. You’ll still be feeling pain.
Worsening Symptoms
If your tear isn’t treated, the condition will get progressively worse. You’ll experience:
- Worsening pain
- Tingling
- Numbness in the limbs/affected area
- General discomfort
- Bulging Disc
If you notice symptoms worsening, you should definitely see a doctor that can diagnose an annular tear.
Diagnosis
On that topic, let’s look at how you can diagnose an annular tear. If you have any or all of the above symptoms, there’s a chance that it’s an annular tear. The likelihood that your pain is an annular tear increases if it’s lower back pain, if you’re older, if you’re overweight, and if you have all of the symptoms listed.
However, to get an official diagnosis you’ll need to see a doctor. They’ll do a full work-up and will probably order an MRI. An MRI will be able to definitively show an annular tear (if that’s what you have).
The doctor can also use a CT scan or a discogram to determine the exact location of the tear.
Treatment Options
If you do have an annular tear, there are several treatment methods. You’ll probably start conservatively in order to avoid surgery: pain medication, anti-inflammatories, weight loss regimens, physical therapy, etc. Annular tears can take up to 2 years to fully heal.
Only when these treatment methods fail, or if your condition is worsening, will a doctor recommend surgery. There are traditional surgery options, endoscopic surgical techniques, and even some experimental stem cell treatments you can try.
Contact Us for More Information
If you have an annular tear, it can progress into a serious and painful condition. Any sort of consistent or recurring back pain should be discussed with a doctor as soon as possible to rule out any serious condition and to get you started on a treatment plan as soon as possible.
Contact us to set up an appointment or to ask any other questions you have.