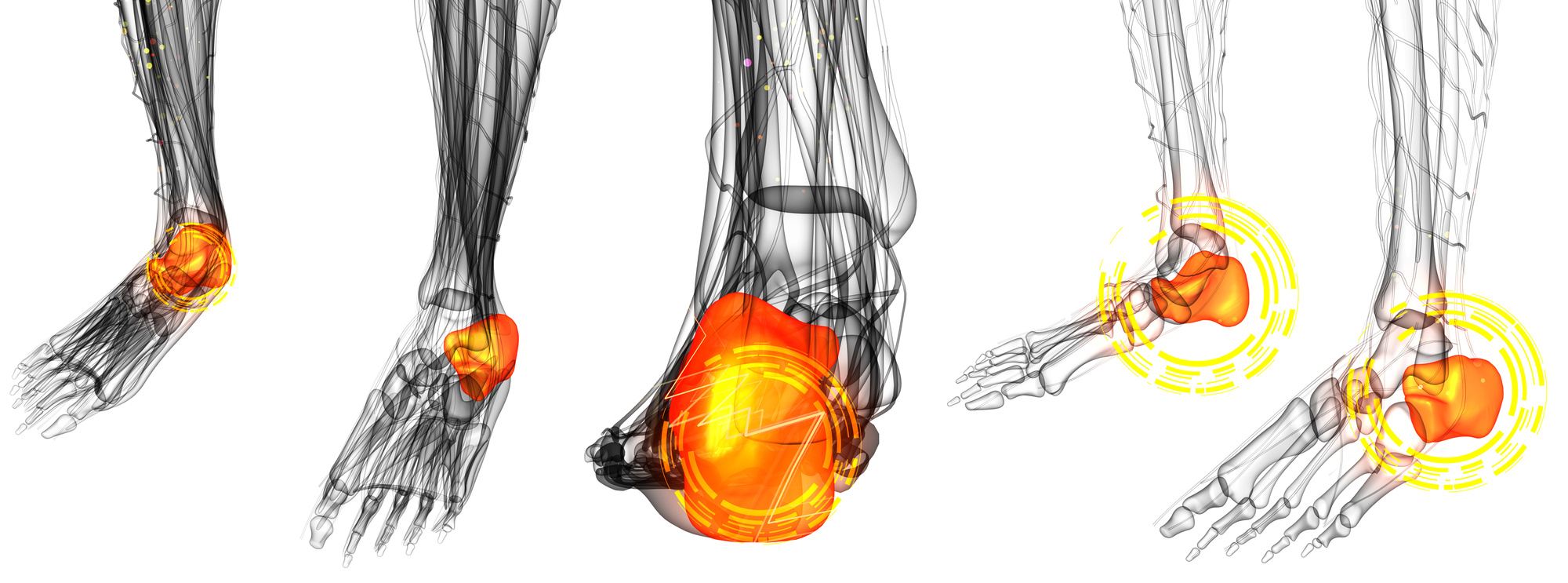
Bone Spurs: What Are They and Where Do They Come From?
Bone spurs can occur all throughout the body, including our hands, feet, spine, and any other joints within the body. However, you may or may not notice they’re there.
So what are bone spur symptoms, what causes them, and can they be removed? These are all common questions we receive from patients who receive a diagnosis, which is why we put together one cohesive blog to answer them all.
What are Bone Spurs?
A bone spur is when additional bone growth develops along the edges of your bones. Typically they occur around the areas where two bones join together, such as your joints or between the vertebrae in your spine.
They usually develop in response to wear and tear between your joints. Whether they’re harmful or not simply depends on how they grow and whether or not they impact the mobility of your bones.
What Causes Bone Spurs?
The most common cause of bone spurs is osteoarthritis.
Osteoarthritis is a degenerative bone disease that affects around 27 million Americans. Those with osteoarthritis experience a breakdown in the cartilage between the joints, which leads to friction between the bones.
This causes a host of different problems, including swelling, joint pain, and reduced mobility.
However, osteoarthritis isn’t the only cause of bone spurs. With age, injury, or wear and tear, the spine can develop spondylolithesis. Spondylolithesis is when an individual experiences damage or develops weakness in the facet joints and discs within the spine.
If this weakness is left untreated and continues to develop, it can lead to instability within the spinal structure. This creates stress within different parts of the spine, including the tendons, discs, and ligaments.
The body responds to this form of stress with new bone growth in an attempt to bring stability back to the spine. However, the development of these bones spurs can lead to other problems, including compression and pinched nerves.
Other causes of bone spurs include obesity, overuse of the joints, genetic predispositions, poor diet, and the narrowing of a patient’s spine.
What are the Most Common Bone Spur Symptoms?
As we stated before, some bone spurs may be completely asymptomatic. The only time symptoms occur is when the bones spurs impact the mobility of your joints or exacerbates them in some manner.
The type of symptoms you have depend on where the bone spurs are located.
Common bone spur symptoms include:
- Difficulty bending or extending your leg due to pain within the knee
- Feelings of numbness or weakness in your extremities due to pinched nerves or a pinched spinal cord
- Difficulty controlling your bowels or your bladder due to pressure on your spinal nerves
- Reduced or painful movement in your hip
- Muscle spasms
- Muscle cramps
- Muscle weakness
- Bumps that you can feel under your skin
You may discover these symptoms become exacerbated with exercise or joint use.
It’s important to keep in mind that experience these symptoms is not a guaranteed diagnosis. Because these symptoms can be indicative of other medical conditions or problems, you must receive a proper diagnosis from your doctor.
If you suspect bone spurs, your doctor will likely have you undergo tests in order to confirm or debunk this diagnosis. These tests usually include a physical examination as well as X-rays, CT’s, or MRI’s.
Your doctor may also conduct an electroconductive test to see if there is any nerve damage.
If you have questions about your diagnosis, symptoms, or causes, don’t be afraid to ask your doctor. He or she is responsible for answering any questions you may have regarding your health, treatment options, and any concerns associated with them.
How Do You Treat Bone Spurs?
If your doctor identifies that you have developed bone spurs that require treatment, he or she will provide you with options. Those options can vary depending upon where the bone spurs are located.
Depending upon the severity of your case, this treatment may be as simple as over-the-counter pain relievers to help with the side effects or therapy. In severe cases, you may require surgery in order to remove them.
Therapy options include steroid shots and/or physical therapy.
If you develop bone spurs within the spine, you may be required to undergo pain mapping prior to any surgical procedures. This is where a numbing agent is inserted into the area of the spine where the patient is experiencing pain.
Typically, this will temporarily relieve or stop the pain if your symptoms are caused by bone spurs. However, if your pain continues in spite of non-invasive treatment your doctor may recommend endoscopic foraminotomy.
Endoscopic foraminotomy is different from the more traditional means of bone spur removal. Safer and less invasive, it involves a very small incision as well as the use of a micro camera in order to remove the bone spur compression.
While this may sound indimidating, endoscopic foraminotomy is a much easier procedure than traditional surgery. It only requires a light, twilight sedation, and the incision is approximately the size of a fingernail.
This means less post-op pain and a significantly decreased recovery time for the patient. It is highly recommended for patients who require a spinal surgery in order to remove bone spurs causing nerve compression.
Explore Your Options for Bone Spur Removal in the Spine
If you have tried the more conservative options to bone spur treatment, but are still suffering from bone spur symptoms in the spine then it may be time to consider surgical options.
Make sure that you select a spinal surgeon with a good reputation and positive testimonials. Quality matters, especially when it comes to any sort of operation on the spine.
This area of your body houses multiple nerves and nerve endings that a good surgeon navigates with the utmost care. Careless or improper execution can lead to serious, and possibly permanent side effects.
If you are a patient within the Hackettstown or Newton, New Jersey area, give us a call. Dr. Carl Spivek is the President of Executive Spinal Surgery P.C. and he specializes in minimally invasive spinal surgeries.
These surgeries are safer and easier on the patient, making it the best available option today.