Back Pain in Young Adults
Causes of Back Pain in Young Adults
Back pain is a common complaint among adults, and it can affect people of all ages. While it may be more prevalent in older adults, back pain can also affect young adults. In fact, studies show that nearly 80% of adults experience back pain at some point in their lives.
Back pain in young adults can be caused by a variety of factors, including poor posture, a sedentary lifestyle, sports injuries, or accidents. It can also be the result of underlying medical conditions such as scoliosis, herniated discs, or spinal stenosis.
One of the most common causes of back pain in young adults is poor posture. Many young adults spend a significant amount of time sitting at a desk or using electronic devices, which can cause them to develop a slouching posture. This can put pressure on the spine and lead to back pain. To prevent this, it is important to maintain proper posture while sitting and standing.
A sedentary lifestyle can also contribute to back pain in young adults. A lack of exercise and physical activity can lead to weakened muscles and a loss of flexibility in the spine, which can make it more susceptible to injury. Incorporating regular exercise into your daily routine can help strengthen the muscles in your back and reduce the risk of developing back pain.
Sports injuries are another common cause of back pain in young adults. Activities such as football, basketball, and weightlifting can put a lot of stress on the back, which can lead to injury. It is important to use proper technique when performing these activities and to wear proper protective gear to prevent injury.
Accidents such as falls or car accidents can also cause back pain in young adults. Even a minor accident can cause injury to the spine, leading to back pain. It is important to seek medical attention if you have been involved in an accident and are experiencing back pain.
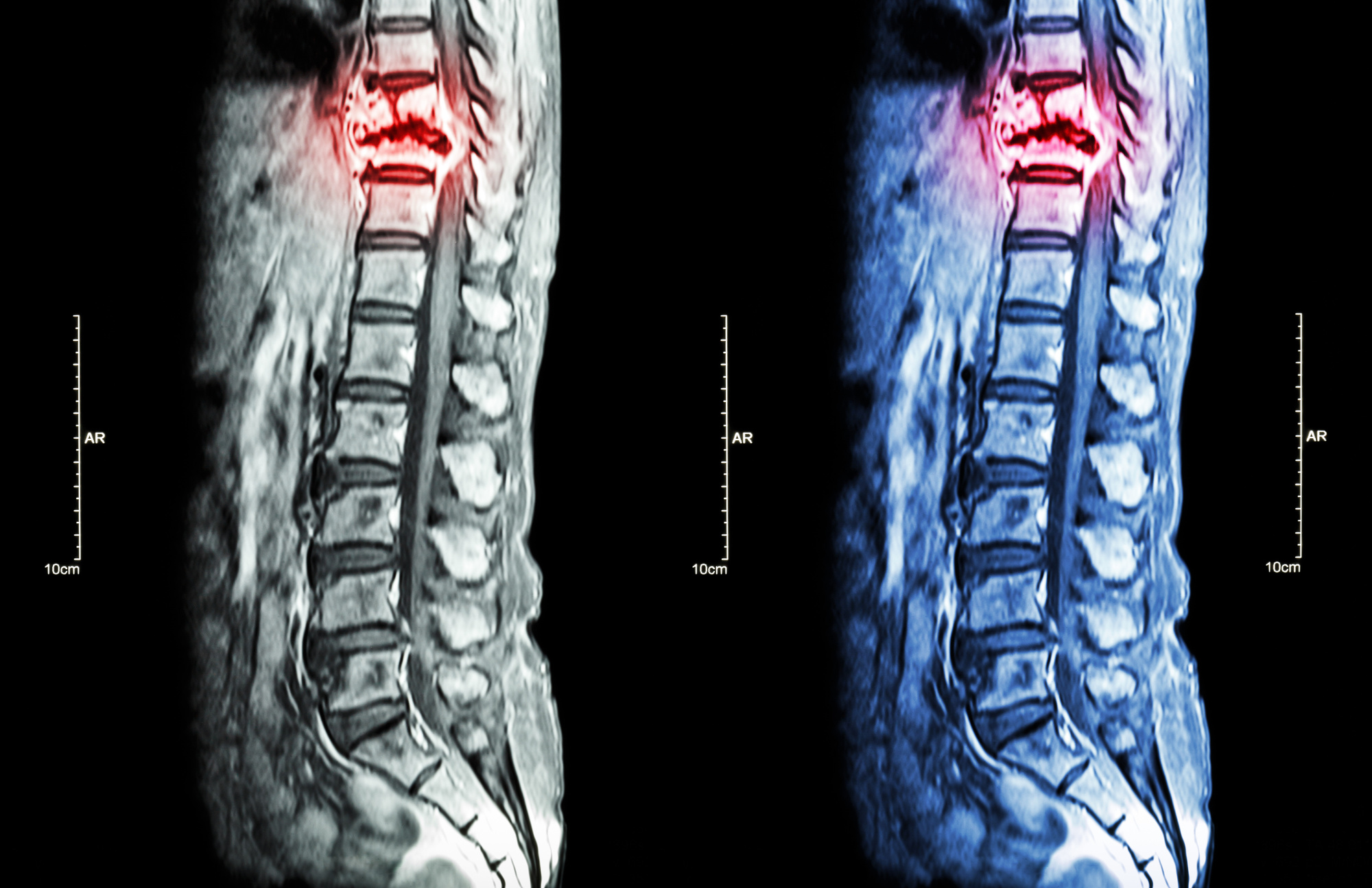
Medical conditions such as scoliosis, herniated discs, and spinal stenosis can also cause back pain in young adults. These conditions can be diagnosed by a healthcare professional and may require treatment such as physical therapy, medication, or surgery.
In general, there are several things you can do to prevent back pain in young adulthood. Maintaining proper posture, incorporating regular exercise into your routine, using proper technique when performing physical activities, and seeking medical attention if you experience pain or discomfort are all important steps you can take to reduce the risk of developing back pain.
In conclusion, back pain in young adults is a common issue that can be caused by a variety of factors. Maintaining proper posture, incorporating regular exercise into your routine, using proper technique when performing physical activities, and seeking medical attention if you experience pain or discomfort are all important steps you can take to reduce the risk of developing back pain. If you are experiencing back pain, it is important to seek medical attention to determine the underlying cause and receive appropriate treatment.
Dr. Carl Spivak, MD at Executive Spine Surgery is a neurosurgeon based in Newton, New Jersey. He specializes in treating back pain regardless of the patient’s age with endoscopic spine surgery. To find out more about our facility, click here.